Potential Drug-drug Interactions Analysis in Children Out-patients with Bronchopneumonia Medication Prescriptions
Abstract
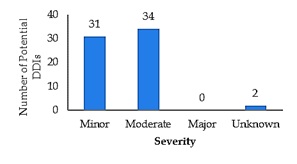
Drug-drug interactions (DDIs) is defined as the alteration of efficacy and toxicity of some drugs in the presence of other drugs. In the treatments of bronchopneumonia in outpatient settings, there is a lack of documentation of DDIs. This study was aimed to observe the potential DDIs on the prescriptions of children with bronchopneumonia. An observational and cross-sectional study was conducted on outpatient children with bronchopneumonia prescriptions during 2017. Potential for DDI was identified by online drug interaction checkers. The potential DDI then classified based on its severity (minor, moderate, and major) and mechanism (pharmacokinetic and pharmacodynamic). Among 86 prescriptions analyzed, potential DDIs observed at 48.84% of it. Of that, there were 67 potential DDIs where 72.34% of it were categorized as moderate. The majority of potential DDIs was pharmacodynamic interaction (76.12%) with the most frequently involved drug pair was Ephedrine-Salbutamol (29.85%). Children outpatients with bronchopneumonia are at risk of potential DDIs, especially to minor and moderate potential DDIs. Prescriptions screening for potential DDIs followed by monitoring of therapeutical effects and associated adverse drug events will optimize patient safety.
Full text article
References
Chang C.C., Cheng A.C., & Chang A.B. (2014). Over-the-counter medications to help reduce cough for children and adults on antibiotics for acute pneumonia. Cochrane Database of Systematic Reviews, 3, CD006088. doi:10.1002/14651858.CD006088.pub4
Dechanont, S., Maphanta, S., Butthum, B., & Kongkaew, C. (2014). Hospital admissions/visits associated with drug-drug interactions: a systematic review and meta-analysis. Pharmacoepidemiology and Drug Safety, 23(5), 489–497. doi:10.1002/pds.3592
Harris, M., Clark, J., Coote, N., Fletche, P., Harnden, A., McKean, M., & Thomson, A. (2011). British Thoracic Society guidelines for the management of community acquired pneumonia in children: update 2011. Thorax, 66(Suppl 2), 1-23. doi:10.1136/thoraxjnl-2011-200598
Ismail, M., Noor S., Harram U., Haq I., Haider I., Khadim F., Khan Q., Ali Z., Muhammad T., & Asif M. (2018). Potential drug-drug interactions in outpatient department of a tertiary care hospital in Pakistan: a cross-sectional study. BMC Health Services Research, 18(1), 762. doi:10.1186/s12913-018-3579-7
Kardalas, E., Paschou, S.A., Anagnostis, P., Muscogiuri, G., Siasos, G., & Vryonidou, A. (2018). Hypokalemia: a clinical update. Endocrine Connections, 7(4), 135-146. doi:10.1530/EC-18-0109
Khalilian, M.R., Fayezi, A., Alisamir, M., & Khorasani, N.M. (2016). Effect of Ventolin on QTc in children with respiratory distress. Journal of Cardiovascular and Thoracic Research, 8(2), 83-85. doi:10.15171/jcvtr.2016.16
Kulkarni, V., Bora, S.S., Sirisha S., Saji, M., & Sundaran, S. (2013). A study on drug–drug interactions through prescription analysis in a South Indian teaching hospital. Therapeutic Advances in Drug Safety, 4(4), 141–146. doi:10.1177/2042098613490009
Loya, A.M., Gonz´alez-Stuart, A., & Rivera, J.O. (2009). Prevalence of polypharmacy, polyherbacy, nutritional supplement use and potential product interactions among older adults living on the United States-Mexico border: a descriptive, questionnaire-based study. Drugs and Aging, 26(5), 423–436. doi:10.2165/00002512-200926050-00006
Nasralla, H.A.A., Al-Hilaly, K.A., & Alghabban, S.I. (2010). Drug induced Hypokalemia: A Retrospective Study. New Iraqi Journal of Medicine, 6(1), 22-26.
Noor, S., Ismail, M., & Ali, Z. (2019). Potential drug-drug interactions among pneumonia patients: do these matter in clinical perspectives? BMC Pharmacology and Toxicology, 20, 45. doi:10.1186/s40360-019-0325-7
Palleria, C., Di Paolo, A., Giofre, C., Caglioti, C., Leuzzi, G., Siniscalchi, A., De Sarro, G., & Gallelli, L. (2013). Pharmacokinetic drug-drug interaction and their implication in clinical management. Journal of Research in Medical Sciences, 18(7), 601-610.
Patel, P.S., Rana, D.A., Suthar, J.V., Malhotra. S.D., & Patel, V.J. (2014). A study of potential adverse drug-drug interactions among prescribed drugs in medicine outpatient department of a tertiary care teaching hospital. Journal of Basic and Clinical Pharmacy, 5(2), 44-48. doi:10.4103/0976-0105.134983
Salpeter, S.R, Ormiston, T.M., & Salpeter, E.E. (2004). Cardiovascular effects of beta-agonists in patients with asthma and COPD: a meta-analysis. Chest, 125(6), 2309-2321. doi:10.1378/chest.125.6.2309
Shetty, V., Chowta, M.N., Chowta, K.N., Shenoy, A., Kamath, A., & Kamath, P. (2018). Evaluation of Potential Drug-Drug Interactions with Medications Prescribed to Geriatric Patients in a Tertiary Care Hospital. Journal of Aging Research, 2018, 5728957. doi:10.1155/2018/5728957
Somogyi-Végh, A., Ludányi, Z., Erdős, Á., & Botz, L. (2019). Countrywide prevalence of critical drug interactions in Hungarian outpatients: a retrospective analysis of pharmacy dispensing data. BMC Pharmacology and Toxicology, 20(1), 36. doi:10.1186/s40360-019-0311-0
Vaidhun, B.H. & Sathish, A. (2011). Out-patients Prescriptions are Safe from Drug Interactions or Not: A Pilot Study Report. Indian Journal of Pharmaceutical Sciences, 73(5), 590-592. doi:10.4103/0250-474X.99024
Zec, S.L., Selmanovic, K., Andrijic, N.L., Kadic, A., Zecevic, L., & Zunic, L. (2016). Evaluation of Drug Treatment of Bronchopneumonia at the Pediatric Clinic in Sarajevo. Medical Archives, 70(3), 177-181. doi:10.5455/medarh.2016.70.177-181
Authors
Copyright (c) 2020 Ilil Maidatuz Zulfa, Fitria Dewi Yunitasari, Susanty Kartika Dewi

This work is licensed under a Creative Commons Attribution-ShareAlike 4.0 International License.
This work is licensed under a Creative Commons Attribution-ShareAlike 4.0 International License.
Authors continue to retain the copyright to the article if the article is published in the Borneo Journal of Pharmacy. They will also retain the publishing rights to the article without any restrictions.
Authors who publish in this journal agree to the following terms:
- Any article on the copyright is retained by the author(s).
- The author grants the journal the right of first publication with the work simultaneously licensed under a Creative Commons Attribution License that allows others to share work with an acknowledgment of the work authors and initial publications in this journal.
- Authors can enter into separate, additional contractual arrangements for the non-exclusive distribution of published articles (e.g., post-institutional repository) or publish them in a book, with acknowledgment of their initial publication in this journal.
- Authors are permitted and encouraged to post their work online (e.g., in institutional repositories or on their websites) prior to and during the submission process. This can lead to productive exchanges and earlier and greater citations of published work.
- The article and any associated published material are distributed under the Creative Commons Attribution-ShareAlike 4.0 International License.